“Gun cleaner shoots self” — Ottawa Sun headline, Jan. 12, 2011
NOTRE-DAME-DE-LA-SALETTE, Que. — On the mantel inside the Desjardins house, which hugs Lac de l’Argile, a mountain lake about an hour’s drive northeast of Ottawa, there are no framed photos of Maurice Desjardins taken after what the family calls only “the accident.”
There’s a picture of Maurice and his wife Gaétane holidaying with friends in Playa del Carmen a year earlier, and a sepia-toned photo taken on their wedding day 44 years ago that still makes Gaétane’s heart “go bump, bump, bump.” Maurice was “so nice,” she says, meaning, so handsome.
Eight years ago Maurice accidentally blew that handsome face off with a hunting rifle, and no matter how hard the doctors tried to reconstruct something, anything resembling normal, he was left with two holes where his nose used to be and a mangled, puckered mouth that couldn’t close and that made him look like a rendition of Edvard Munch’s The Scream. He had to breathe through a tracheostomy, a surgical hole in his throat.
Then, last May, a team of nine surgeons at Montreal’s Maisonneuve-Rosemont Hospital lifted the face off a brain-dead man and laid it over Maurice’s skull like a rubber mould. Neck, chin, mouth, cheeks, nose — the face came off as one piece, all the bones of the upper face, the maxilla, the entire mid-face and jaw. The surgeons connected the artery and vein from the donor’s face to Maurice’s neck, removed the clamps to restore blood flow and today that reanimated face is starting to move.

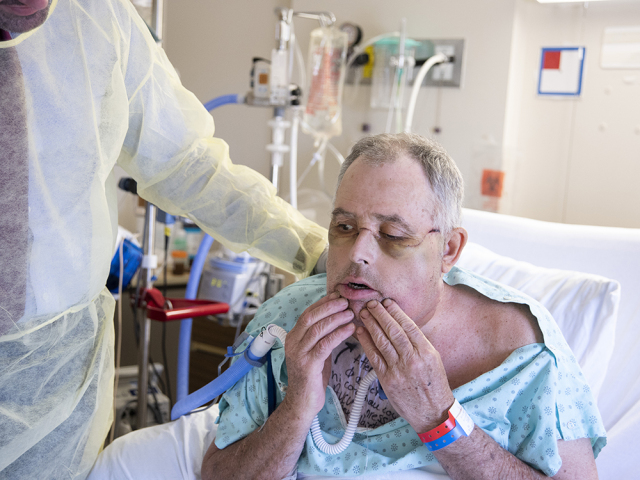
The flesh is smooth, the cheeks puffy. The sensory nerves are recovering. His lips can move. Pinch his cheeks and, though the sensation is a little dull, Maurice can feel it. He can feel the inside of his mouth, or rather, the donor’s mouth. If something touches his face, he knows whether it’s hot or cold. When he shaves, he can feel the blade moving over stubble. He could never grow a beard before.
The motor function is coming back, too, though it’s hard to appreciate it, because his mouth hangs wide open. It’s often almost impossible to understand him. He’s fallen back on the facial exercises he was taught in rehab, because of complications related to the drugs that are keeping his body from rejecting a stranger’s face.
His eyes are still his own. They’re big and bright and lively. He’s there, behind those eyes — behind a face that looks astonished, because his mouth hasn’t fully closed. “I’m still the same guy,” he says. When he smiles, his left eyebrow lifts, one corner of his lip ever so slightly, too. Dr. Hélène St. Jacques, the psychiatrist who worked with Maurice for two years before his historic face transplant, the first in Canadian history, says what is most important for face recognition is the eyes. The forehead is Maurice’s, too. So are his ears. His nose is the donor’s, but the surgeons narrowed the tip and nostrils, to make it different, more Maurice’s.
I just want him to be happy. And I think we’re getting there
After the landmark surgery, on which the Post reported exclusively in English Canada, people stopped Maurice on the streets — here, in this rural Quebec village nestled among the hills by the Lièvre River, and in Montreal, where Maurice and Gaétane still travel frequently for follow-up medical care. Everywhere, people stopped him. It’s a marvel, a miracle, they said. “Can I take your picture?” Dr. Daniel Borsuk, the plastic surgeon who led the team of more than 100 medical, nursing and support staff, became a medical “superstar.”
“I think if you want to talk medically, things have been a success,” Borsuk says as he reflects back over the first year. “Things,” he says, might have shifted a little. Like the plates that are holding Maurice’s jaws in place. “We might have to put in different plates. It’s not a big thing, but it’s frustrating,” says Borsuk, a perfectionist. But with adjustments, with “little revisions” — injecting a little fat here, removing two back teeth — Maurice’s jaw should close within a month or so.
The doctors have delivered on other things: Today, the man who lived without a face for seven years is able to walk around in public without a hospital mask. He no longer has a tracheostomy. His new face, says Maurice, 65, has given him a second chance at life, a regained second identity. But it’s brought other things, too, including serious financial strain. He and Gaétane are struggling to pay for medications not covered by insurance, and for gas and travel to and from Montreal for the constant follow-up and monitoring. They recently posted a GoFundMe page. So far, they have raised just $ 100.
Maurice still can’t eat a full meal through his mouth. A feeding tube is still supporting him. He takes 15 different medications, including anti-rejection drugs needed to beat back his immune system but that leave him vulnerable to infections, cancer, diabetes and a shortened life. He’s had an infection of his eyelids, and the skin on one thigh. In March he underwent emergency surgery for diverticulitis, where inflamed or infected pouches form on the colon wall. One day one of the pouches ruptured, spilling intestinal content into Maurice’s gut. Gaétane rushed Maurice to the hospital in Montreal, convinced he was dying. “He wasn’t answering me anymore; he wasn’t talking anymore. I was driving fast.” Police stopped her just outside Montreal. “I said, ‘Please, come with me, take me the way, bring my husband to the hospital, he’s going to die.” Instead, she was given a $ 325 speeding ticket. When Borsuk saw Maurice in the hospital, “I called intensive care, I called the general surgeon and they operated on him that night.” Maurice now has a temporary colostomy. The doctors expect to remove it in three to six months and put his bowels back together. For Maurice, there’s no more intestinal pain. But it was one of several setbacks.
“His life before is not like his life now, with all the medical visits,” Borsuk says. “It takes some time to adjust to it. He’s impatient; I’m impatient. We want it to be perfect right away and unfortunately that’s not how it works. It’s going to take time to establish a normal life. It’s not just in this case — it’s in all (face) transplants.”
“I just want him to be happy. And I think we’re getting there, we’re getting there.”
It’s going to take time to establish a normal life
Maurice now belongs to a new generation of organ recipients known as vascularized composite allotransplantation, or VCA, patients. People whose transplants involve not just the transfer of a stranger’s single organ — a kidney, a liver — but their muscle, nerve, bone, tendons and skin. Body parts like faces, arms and hands, as well as “genitourinary structures” like a penis or uterus. Some 40 face transplants have been performed worldwide since 2005, and 100 arms. Despite early skepticism, and serious questions about whether it was moral to even attempt them, “the field has demonstrated feasibility and success,” according to a recent paper in the journal, Transplantation. Now, as they become more common, as more centres like Montreal mull performing them, VCA’s are raising significant ethical challenges, including how to predict who is going to do well, and who isn’t, and are the benefits of these non-life-saving procedures sufficient to justify the risks, and expense?
“There are still lots of challenges, obviously. It’s not a walk in the park,” says ear-nose-and-throat surgeon Dr. Akram Rahal, who was a member of the team that gave Maurice another man’s face last May. “With any surgical or medical breakthrough, we always have to think about, why are we doing it? What are the benefits? The patient has to be at the centre of the decision. We can’t lose focus of that.”
***
“Once you are satisfied that the bore is clean, you can leave the bore dry if you are going to shoot the same day. However, if you have to store the gun overnight or for a longer period of time, you will need to protect the bore from rust. Run a patch soaked with oil down the bore.” — NRA Family: How to Clean Your Gun
On the morning of Jan. 10, 2011, Maurice took his hunting rifle into his garage. He had last shot it the month before, hunting caribou in James Bay, and he wanted to clean it. It was just after 9 am. His daughter-in-law, Stephanie, was home in the apartment above the garage.
Maurice had stored the gun while it was still loaded. He says he removed the bullets before cleaning the rifle, but one bullet, unbeknownst to him, was stuck in the chamber. “I cleaned it. I oiled it, and it was too oily,” Maurice says. The gun slid out of his hands, he says. The butt hit the floor, the firing pin fired and the bullet entered his neck. He points his index finger under his chin to show me. It was a classic “avulsion” injury. It wasn’t a neat, straight hole. Instead, that striking projectile carved a torturous pathway through his face. The jaws, the mouth, the nose, the whole anterior part of the face were pulled off.
It’s not only a miracle he didn’t die, miraculously, Maurice remained conscious. He stood up, grabbed a broom and bashed on the ceiling with the handle — thump, thump, thump. When Stephanie came downstairs, there was a hole in the middle of Maurice’s face and he was choking on the shattered pieces of teeth. Stephanie fished out all the teeth she could and ran to the neighbours to call 911, and when police arrived Maurice was on the floor. The first officer on the scene thought he was dead. “But then he was up and the police said, ‘Holy geez, he’s not dead,’” Gaétane remembers Stephanie telling her. “But his face wasn’t there no more.”
Gaétane was in Cuba with friends. She was getting ready for dinner when the phone rang. The sergeant on the other end of the line told Gaétane something had happened to her husband. “I said, ‘What? What? Is he dead?’ He said, ‘He’s not dead, but he’s not doing good. He’s had an accident with his gun.’ I just fell down on the floor.”
She flew home, and when she arrived at the hospital, Maurice was in intensive care. His face, what was left of it, was swollen and swaddled in bandages. Only his eyes were showing. “I saw his eyes and I said, ‘Yes, it’s him.”
Maurice spent nine months in hospital. He couldn’t speak for a year-and-a-half. A police investigation determined the gun was accidentally fired.
Dr. Tareck Ayad and Rahal were the first to operate on Maurice’s face. They did numerous reconstructions, all with the goal of restoring some kind of function, “and when I say function, I mean eating and being able to speak and eventually get him to breathe without a tracheostomy,” Ayad says. Before his face transplant, Maurice could only speak by pressing over the tracheostomy opening with his fingers. He lost his small roofing business. When he left his house, people stared.
Last spring’s face transplant, which began at dawn on May 10, took 30 hours. It involved nine surgeons who had spent two years practising on cadaver heads. It took 17 hours to remove Maurice’s face, because of the multiple reconstructions. “We had to basically dismantle all the work we had done over the years,” Rahal says. “This was, for us, kind of a grief. We had to dismantle all that we had done to be able to offer him a new face.”
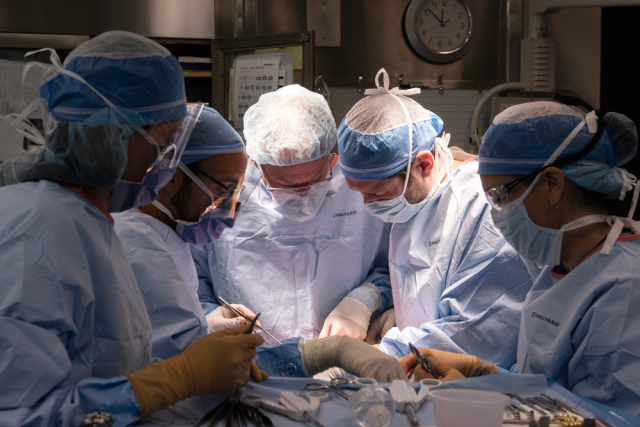
There were more than 100 people involved. And, Gaétane believes, “God was there. God was in that room, too.”
Maurice is now slowly regaining his strength. He’s lost 32 kilograms since the transplant. He’s four years sober. He had to stop drinking before the transplant. “He didn’t want to live anymore, that’s why he was drinking, and Dr. Borsuk said, ‘You have to stop everything. Everything,’” Gaétane says. On our visit, Maurice plays with his dogs, Bella and Cocotte. He dabs at his eyes, and wipes his mouth. The living room and kitchen are filled with bottles of pills and lotions, syringes and latex gloves. The drugs keeping his face alive have to be administered three, four times a day. But Maurice has accepted his face, he says. There seems no issue of “challenged identity.” The donor isn’t somehow living on in his transplanted chin, nose and mouth. The face, Maurice says, is his.
Does it still feel like a marvel, a godsend? “Ah, oui. Oh, yes.” The man whose face he wears was in his 40s. In addition to his face, the donor’s family consented to harvesting his pancreas, heart and other organs. His liver saved a dying baby. What would Maurice say to the mother of the donor if he could? He pauses. His eyes water. “Thank you,” he says. “And I would hug her.”
• Email: skirkey@postmedia.com | Twitter: sharon_kirkey



