 Most new cancer treatments haven’t been proven to help patients live longer or feel better. Instead they delay the growth of tumors — which may be faster to measure but doesn’t necessarily indicate a tangible benefit for patients.
Most new cancer treatments haven’t been proven to help patients live longer or feel better. Instead they delay the growth of tumors — which may be faster to measure but doesn’t necessarily indicate a tangible benefit for patients.
But you wouldn’t grasp that sobering fact from some recent news coverage:
- A headline in the UK’s Telegraph about the drug olaparib (Lynparza) read: “Revolution’ in prostate cancer care as off-label breast cancer drug doubles survival.”
- A Miami Herald story said the drug veliparib could “help at least 30 percent more patients” and have “wide-ranging implications” in the treatment of ovarian cancer.
- Healthline called the approval of atezolizumab (Tecentriq) “big news” with a “substantial survival benefit” for people with triple-negative breast cancer.
“Revolution?” “Wide-ranging?” “Big news?”
Such hype can fuel unrealistic expectations of cancer treatments, experts said.
That’s because each of these stories dealt with an often-misunderstood surrogate endpoint that researchers call progression-free survival (PFS). (You can you can read more about the limitations of surrogate endpoints here.)
Despite including the word “survival,” the term PFS doesn’t indicate how long patients will live. It’s generally defined as the time that it takes for tumors to grow beyond an arbitrary amount, or for new ones to appear on a scan. That metric doesn’t necessarily tell you anything about overall survival.
Yet none of the stories explained those limitations, and two misled readers by saying a drug improves “survival.”
PFS needs to be better explained
PFS numbers can sound impressive. The Herald, for example, reported that patients who got veliparib “had a median time of progression-free survival of 34.7 months, compared to 22 months for those who didn’t receive the medication.”
But most patients “have no idea what progression-free survival means prior to entering the world of medicine. It is one of those classic surrogate endpoints that is meaningless to patients until we explain it,” said Adam Cifu, MD, an internist and professor of medicine at the University of Chicago, via email.
Alyson Haslam, PhD, a senior research scientist at Oregon Health & Science University, said in an email: “Progression-free survival is more often about what’s going on with the tumor during treatment and less about meaningful benefit to the patient, and this message often gets missed in news stories.”
For researchers PFS serves a useful, if controversial, purpose: allowing for shorter studies with fewer patients. In the last decade it’s become the norm in cancer trials.
“There are a lot of patient advocacy groups who do push for that because they want access to drugs for diseases that don’t have effective treatments,” said Michelle Tregear, a breast cancer survivor who is the director of education and training at the National Breast Cancer Coalition, an advocacy group whose mission is to end breast cancer.
But Tregear added, “The media are as confused as the public is about what PFS actually means.”
For journalists, surrogate endpoints such as PFS can be “important to report on — sometimes it’s all we have,” said UCLA breast surgeon Deanna Attai, MD. But Attai and others noted that caveats such as the lack of an overall survival benefit should be included in the discussion.
Weak predictors of overall survival
News coverage should acknowledge a growing body of evidence cautioning about the use of PFS in cancer research. For example:
- An analysis co-written by Haslam, that found surrogate outcomes such as PFS are usually weak predictors of overall survival.
- A review in JAMA Oncology showed no link between PFS and quality of life.
- A literature review published in JAMA Oncology showed it’s unclear patients with advanced cancer understand or value PFS.
A BMJ editorial published in September cited six examples of treatments that improved surrogate markers such as PFS but didn’t help patients live longer. It noted drugs that lengthen PFS might make patients worse off. In June researchers announced the drug venetoclax appeared to hasten the death of myeloma patients, though it nearly doubled PFS compared with a control.
Haslam said while it “would be nice to measure overall health with a simple, single measurement, our research and the research of others shows that PFS is often a poor marker for outcomes that are most important to the patient, such as living longer or better quality of life during and after treatment.”
Would a new name help?
Some say the term PFS has generated so much confusion that it ought to be renamed.
Vincent Rajkumar, MD, professor of medicine at the Mayo Clinic in Rochester, Minn., said PFS is misleading because it “sends a message that it’s a great victory.”
“It’s as if you are running a 5K race and you are declaring the winner at the 3K mark,” he said. “You should not be giving the illusion of certainty when there is none.”
On Twitter Rajkumar called on medical journals to remove the word “survival” from the term.
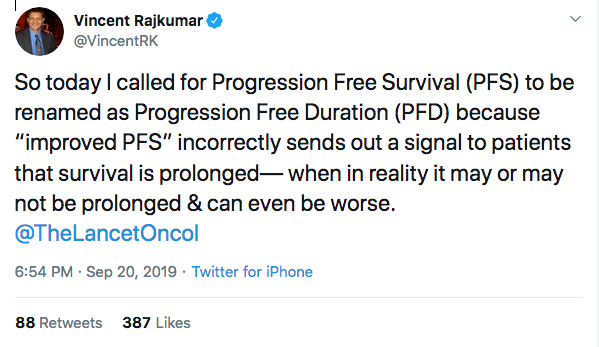 In a subsequent tweet, he expanded on why PFS is problematic:
In a subsequent tweet, he expanded on why PFS is problematic:
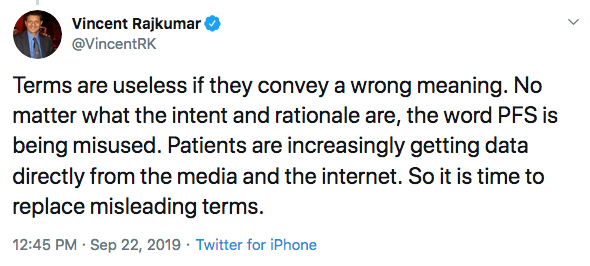 Whether or not “progression-free duration” ever takes hold, it will always be the job of journalists to expose the quality of evidence behind cancer drugs. Some have done an excellent job.
Whether or not “progression-free duration” ever takes hold, it will always be the job of journalists to expose the quality of evidence behind cancer drugs. Some have done an excellent job.
Among them: a review by Peter Loftus of the Wall Street Journal published in July found that of 42 fast-tracked cancer drugs the FDA approved from 2015 through 2018, “just 19% had proof upon approval they significantly prolonged overall survival.” That report bolstered reporters’ John Fauber and Elbert Chu findings in their 2014 piece in the Milwaukee Journal Sentinel, FDA approves cancer drugs without proof they’re extending lives.
How journalists can do better
News stories can go beyond cursory descriptions that might suggest to readers a benefit that doesn’t exist. The Telegraph said PFS is “the period during which the cancer does not get worse.” The Herald called it “time where the cancer is not progressing.”
Who wouldn’t want to keep cancer from “progressing” or “getting worse”?
“I think the message that people often get when they read or hear about improved PFS is that survival will be longer or that health deterioration has been halted,” Haslam said. “On the surface this seems like a reasonable assumption, but because we know from research that this is more often not the case, it is important that the reporting of PFS also comes with a better explanation of what this term really means.”
Also useful would be more complete reporting on treatments including costs, adverse effects, and conflicts of interest, said Tregear and Judi Hirshfield-Bartek, a retired oncology nurse who is on the National Breast Cancer Coalition’s board.
The three stories sparsely reported on those areas, which are among HealthNewsReview.org’s 10 criteria for news stories. (Healthline did mention Tecentriq’s $ 13,400-a-month price tag.) Hirshfield-Bartek said the stories all seemed to be “based on a news release,” a promotional statement released by a research institution or drug company.
On the other hand, Rajkumar said journalists could greatly improve their reporting simply by including a line about whether a drug improves overall survival: “That way the investigators who are enthusiastic about the drug are kept honest.”
